Lawmakers’ latest fib about small biz insurance
By Katy Grimes
As the Legislature crammed to clear their plates this week so they could take their summer break, one atrocity after another oozed from the committees in the form of legislation.
One of the worst was SB 1431, which will add to the already heavily regulated health insurance market by prohibiting the sale of stop-loss policies to employers with fewer than 50 employees.
It sounds like a lot of inside baseball, but this group of small employers is already the easy target of heavy regulations and insane California laws. SB 1431 will further penalize this group of innovators, risk takers, and entrepreneurs. Lawmakers have deluded themselves into believing that it’s a good thing.
SB 1431, by Sen. Kevin de Leon, D-Los Angeles, would establish a minimum number of health claims for stop-loss policies issued to employers in the small group health insurance market. And it requires guarantee issue for all employees and dependents, and guarantee renewability of the policy for the small employer.
According to the bill analysis, de Leon said, “SB 1431 will protect consumers in California’s small group market as the Affordable Care Act is implemented.” Beware.
Obamacare
The Affordable Care Act, more commonly known as Obamacare, “puts in motion a number of significant small group market reforms and creates a competitive marketplace through the Exchange,” the bill analysis states. “However, as federal health care reform goes into full effect, there will be incentives for some small employers to self-insure and to purchase stop-loss coverage. The author states this situation could lead to a significant exodus of small employers from the small group market, specifically those employers with young and healthy employees. If this situation occurs, adverse selection could leave in its wake a majority of the state’s small businesses in an insurance pool increasingly subject to skyrocketing premiums, both inside and outside of the Exchange. The author states that even those that self-insure and buy a stop-loss product may soon end up in this pool if the stop-loss carrier decides to drop them.”
But the devil is always in the details. The concern de Leon appears to be showing for small employers should have been blown out of the water by the facts during the Assembly Health Committee hearing on Tuesday. But with State Insurance Commissioner Dave Jones at the hearing, it appeared that no one was willing to challenge the facts.
According to Craig Gottwals, an attorney and insurance expert with BB&T–Liberty Benefit Insurancces Services, Inc., if SB 1431 is passed, the sale of stop-loss policies to employers with fewer than 50 employees will be prohibited by the state if those policies do any of the following:
* Contain a specific attachment point that is lower than $95,000 (an absurdly high amount to mandate for a small employer);
* Contains an aggregate attachment point that is lower than the greater of one of the following:
1. $19,000 times the total number of covered employees and dependents;
2. 120 percent of expected claims;
3. $95,000
“This legislation also erroneously contains language referring to stop-loss carriers as providing ‘coverage’ to individual employees and dependents,” Gottwals said. But that is not what stop loss does. “Stop loss provides a reimbursement agreement for an employer who has undertaken the task of self-insuring his population. The politicians wanting to further dismantle freedom and play the harp stings of victimhood undoubtedly used such Orwellian sounding terminology on purpose,” Gottwals said.
This law prohibitively restricts the most innovative and diligent of California’s smaller entrepreneurial businesses by taking away their ability to use creativity and customization to do what is best for their employees, by ramming an over-priced, one-size-fits-all Obamacare-esque approach to health coverage, all the way down to a 2-person company.
Limited choices
Gottwals said what’s left for small employers is limited. “So now a California employer who is intelligent, willing to take some risk, and be creative, will be further penalized and presented with three choices:
1) Stop offering healthcare altogether, which will already be rather enticing in 2014 when the state exchange is set up and the employer has the political cover of “encouraging” use of Obama’s governmental exchanges.
Also, remember, employers under 50 employees will not pay the employer mandate fines under Obamacare. Hence, an employer can cease offering benefits, and encourage its employees to take advantage of the subsidies available to those making up to four times the federal poverty limit, approximately $90,000 for a family of four.
2) Move out of state to a jurisdiction that does not detest small business and entrepreneurship.
3) Buy an overpriced, first dollar benefit HMO or PPO. But note, if the employer could afford this option, they would have almost certainly done so already as self-funding is much more difficult, takes more time and has more risk involved. So which employers are self-funding under 50-lives now — those in rural areas with no simple access to an HMO. Those employers will be particularly harmed.”
What is really going on here?
California already controls and highly regulates the under 50-employee insurance market for all fully insured products.
The federal government has now taken large control over the over-50 market with Obamacare.
Self-insuring is the only remaining frontier where an employer can extract itself from the myriad of state-regulation as well as some of the dictates of Obamacare (such as the medical loss ratio mandates, possible avoidance of the future Cadillac Tax, and allowance for medical underwriting).
Self-insuring in the under-50 market permits an employer to operate under one, reasonable set of federal laws, the Employee Retirement Income Security Act of 1964 (ERISA), without having to also navigate state mandates, and many of the disastrous dictates of Obamacare.
Gottwals said that it is apparent that California wants to take away the few remaining options small employers still have. “This law will almost certainly push small employers to a place where they have to stop offering any health care plan, ultimately bringing California one step closer to a single-payer healthcare plan in our state exchange.”
Related Articles
Affirmative action shakedown of CA insurance industry
July 24, 2012 By Katy Grimes Despite the anti-affirmative action wave that has washed over America, affirmative action policies are
Lawmakers seek soda warning labels
A group of state lawmakers wants to single out “The Coke Side of Life” for a mandatory warning label that
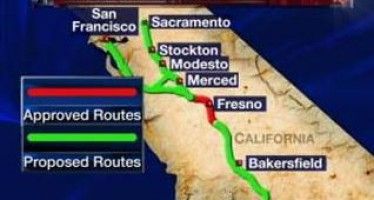
LAO questions legality of plan to use cap-and-trade $ on bullet train
The governor’s just-released 2014-15 budget proposes to spend $850 million from cap-and-trade auction revenue on various projects — including the